Total hip replacement
Total hip replacement is a most effective treatment for arthritis of the hip.
What is it?
A total hip replacement is indicated when pain from your arthritic hip is effecting your ability to perform activities of daily living satisfactorily and when non operative measures such as anti inflammatory medication, activity modification and joint rehabilitation exercises are no longer effective.
Dr. Stening’s preferred method is the anterior approach. Please refer to his surgical technique outlined below.
Total hip replacement is a most effective treatment for arthritis of the hip. It is indicated when pain from your arthritic hip is effecting your ability to perform activities of daily living satisfactorily and when non operative measures such as anti inflammatory medication, activity modification and joint rehabilitation exercises are no longer effective.
Arthritis is where the cartilage that coats the bone wears out and there is bone on bone. This causes pain with movement of the joint. There are many causes of arthritis. Osteoarthritis is the most common. Diagnosis is made by history, physical examination, plain Xrays and sometimes more specialized tests such as MRI.
What’s involved?
Once you have decided to proceed with surgery your surgeon will arrange for pre operative investigations usually organised through pre admission clinic at the hospital. You will need to cease all anti inflammatory drugs and naturopath/herbal medicines 10 days beforehand. Ensure that you have no dental or other medical conditions that may affect outcome of surgery. You may be referred to a general physician. Cease smoking 6 weeks beforehand.
You will usually be admitted to the hospital on the day of your surgery unless you are first on the list in which case the hospital admissions department may organize for you to come in the night before. You will meet the anaesthetist and nurses who will ask you certain relevant questions and the operative area will be shaved and cleaned. There may some more tests organised if deemed necessary.
It is important that you bring in all relevant Xrays as these will be referred to by your surgeon during the procedure.
A hip replacement should reduce your pain considerably, improve your mobility, enable comfortable night’s sleep and generally improve your quality of life.
Podcast: Dr Stening talking about hip conditions and treatment.
Post-Operative Information
Post operatively you will be transferred to the recovery ward. You will have monitors attached and intravenous lines to administer medications. You may also be catheterised. An Xray will be done in recovery to check that the hip replacement is satisfactorily aligned.
On the day following your surgery the drains will usually be removed, you will be sat out of bed and physiotherapist will see you to assist with your mobilising. You will be able to put all your weight on your leg but you will be using aids such as forearm support frame or crutches to assist your walking. Approximately 3 – 5 days post operatively you will either be transferred to a rehab facility or discharged directly home depending on your home circumstances and progress while in hospital.
The timing for post operative visit with your surgeon will be arranged prior to discharge. Usually dissolvable stitches are used so there is no need for removal however you should have a wound check by either your surgeon or local doctor at 2 weeks.
Precautions
- If you have a hip replacement through a posterior approach you must avoid bending your hip and rotating your leg inwards simultaneously for 6 weeks afterwards as there is a risk of dislocation of the replacement with this manoeuvre. These precautions are not necessary with the anterior approach. You should also sleep with a pillow between your legs and avoid sitting on low chairs or toilet seats without a raise during this time.
- Any cuts or scratches on the operated leg need to be dressed adequately to avoid potential infection. If you are having any dental work or other surgical procedures you should advise the surgeon that you have a hip replacement and you should receive antibiotics before and after treatment in order to prevent infection in your replacement.
- As with any major surgery there are risks and complications that may occur.
- General risks are those with the anaesthetic and others due to associated medical conditions. These include allergic reactions to medications, heart attack, pneumonia, stroke, urinary tract infection, renal failure, blood loss requiring transfusion.
- Specific risks associated with the procedure include deep venous thrombosis (DVT), nerve damage, leg length inequality, dislocation of the prosthesis, wound complications and deep infection. The surgical team is very mindful of these risks and measures are taken to reduce the chance of these occurring but cannot be guaranteed. If concerned you should talk to your surgeon however a further consultation may be required.
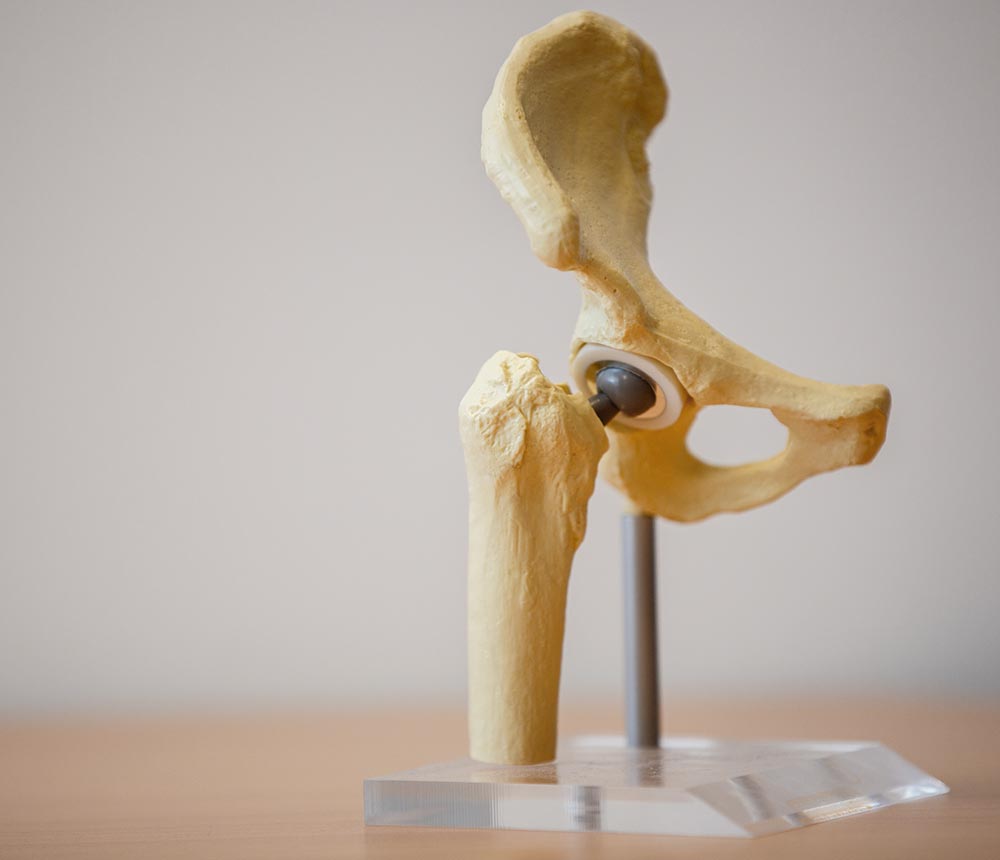
The Hip
The hip joint is formed by the articulation of the rounded head of the femur and the cup-like acetabulum of the pelvis. It forms the primary connection between the bones of the lower limb and the axial skeleton of the trunk and pelvis.
The surface of the femoral head and the acetabulum, where the bones come in contact, is coated by a smooth tissue called articular cartilage. The cartilage, together with a substance called synovial fluid, prevents the bones from rubbing against each other and from becoming damaged.
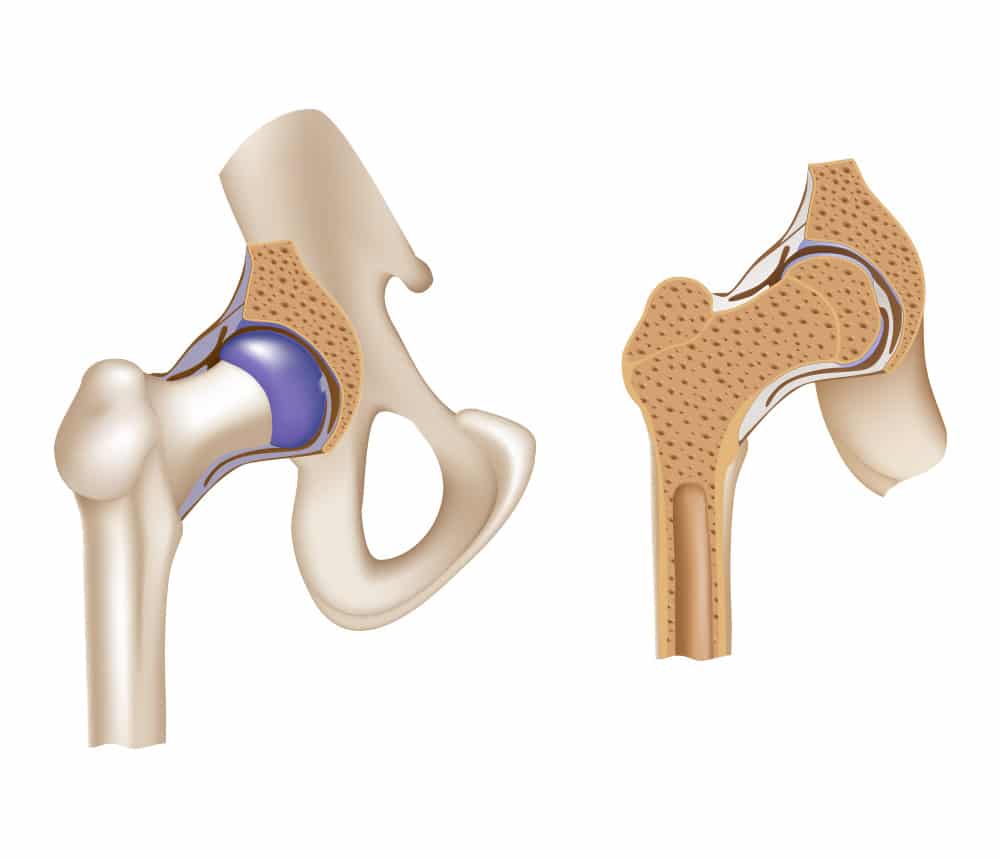
Osteoarthritis of the hip (the most common form of Hip disease)
The main cause of hip joint diseases is the wear of the articular cartilage: osteoarthritis. This wear causes pain, initially only when a load is bearing on the joint but over time it becomes painful more and more frequently eventually leading to constant pain even when resting.
The increase in intensity of the pain is a slow process, sometimes over many years, and can lead to a stiff hip joint.
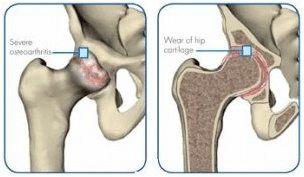
- Hip arthritis typically affects patients over 50 years of age.
- It is more common in people who are overweight, and weight loss tends to reduce the symptoms associated with hip arthritis.
- There is also a genetic predisposition of this condition, meaning hip arthritis tends to run in families.
- Other factors that can contribute to developing hip arthritis include traumatic injuries to the hip and fractures to the bone around the joint
The symptoms of a hip joint problem may include:
- Pain in the hip joint (usually felt in the groin area)
- Referred pain to the thigh and knee
- Limping
- Reduced range of motion
- Muscle stiffness
- Pain when trying to put weight through the leg on the affected side.
Hip replacement is a common treatment for severe osteoarthritis. Successful hip replacement brings dramatic pain relief and improvement in the function of the hip joint.
Total Hip Replacement
Total hip replacement surgery substitutes the damaged bone and cartilage of the joint with polyethylene (a plastic material) or ceramic and metallic components.
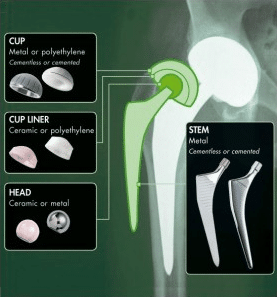
The artificial joint is a spherical articulation, composed of a femoral stem with a head (sphere) and a socket cup (hip socket).
The stem is made of metal (usually a Titanium or Cobalt Chrome alloy or stainless steel), which guarantees a maximum biocompatibility. The femoral head is made of ceramic or metal. The cup is made of polyethylene or metal with a porous surface (which guarantees perfect bone integration). A cup liner, made of ceramic or polyethylene, assures a long life for the artificial joint, even when loaded under stresses.
With almost 70 years of history, total hip replacement surgery is a very common and safe procedure for the treatment of severe osteoarthritis.
The main benefits of a successful total hip replacement are:
- Reduction in hip pain: the pain will be rapidly and dramatically reduced and usually eliminated.
- Recovery of mobility: your hip will function with less effort, almost regaining your original mobility.
- Improvement in quality of life: your everyday activities and your social life will no longer be limited by pain and reduced mobility.
Dr Stening mainly performs the AMIS® (Anterior Minimally Invasive Surgery) approach for total hip replacement procedures because it reduces the risk of injury to your muscles, tendons, vessles and nerves. This means your recovery following surgery will be much more rapid compared to the other surgical approaches that involve cutting the muscle. Although the AMIS® technique may be ideal for total hip replacement surgery not all patients may be suitable for a variety of reasons. Dr Stening will determine this at the time of consultation after he has examined you and reviewed your Xrays.
True Minimally Invasive Surgery (MIS) is characterized by the preservation of muscles and tendons encountered during the surgery to the hip joint capsule and also offers a reduced skin incision. (meaning your scar will be smaller).
The anterior approach AMIS® follows the principles of MIS. Other approaches advertised as minimally invasive (posterior, lateral, or double incision approach) are only reduced skin incision techniques (smaller scar) but are associated with the same muscle and/or tendon injury as “conventional” approaches.
The AMIS® or ‘Anterior approach’, in fact, is the only technique which follows inter-muscular and inter-nervous planes to reduce the risk of injury to muscles, tendons, vessels and nerves.
The AMIS® technique has decreased the incidence of complications when compared to “conventional” techniques and can potentially provide you with the following benefits:
- Decreased Post-Operative Pain: in comparison with “conventional” surgical techniques, the AMIS® approach can reduce the post-operative pain as muscles are not cut.
- Smaller Scar: the skin incision is often shorter than with “conventional” surgery and therefore scar tissue is reduced.
- Prevention of Limping: AMIS® is characterised by a surgical technique that protects the various muscles, blood vessels and nerves encountered during exposure of the hip joint. Minimizing muscle and nerve damage reduces the chances of limping .
- Reduced Risk of Dislocation (separation of the hip ball and socket): The preservation of muscles significantly improves the stability of the hip. The risk of dislocation is minimal and the post-operative limitation of movements, usually prescribed in other techniques, is not necessary. The risk of dislocation is reduced because the AMIS® technique is performed from the front of your body and dislocation is mainly related to posterior hip structure damage.
- Shorter Hospital Stay: The AMIS® technique usually significantly reduces the duration of hospital stay. Dr Stening may still recommend a longer stay, depending on your post-operative condition.
- Less Blood Loss: Preservation of muscles and vessels potentially reduces blood loss. Transfusions are rare, blood clots in the legs (deep venous thrombosis) are potentially less likely.
- Quicker Rehabilitation: Rehabilitation can usually start the day of the operation, or the day after (based on individual post operative conditions) which includes standing up and walking with arm crutches.
- Faster Return to Daily Activities: You usually return to daily activities in a shorter time frame. You may drive when able to get in and out of the car comfortably, have excellent control of your legs and are not taking pain medications. (in most cases this is 8 to 10 days).
