Total and partial knee replacement
Total or partial knee replacement is an effective treatment for arthritis of the knee.
What is it?
A total or partial knee replacement is indicated when pain from your arthritic knee is affecting your ability to perform activities of daily living satisfactorily and when non operative measures such as anti inflammatory medication, activity modification and joint rehabilitation exercises are no longer effective.
Arthritis is where the cartilage that coats the bone wears out and there is bone on bone. This causes pain with movement of the joint. There are many causes of arthritis. Osteoarthritis is the most common.
Diagnosis is made by history, physical examination, plain Xrays and sometimes more specialized tests such as MRI /CT scans.
A knee replacement should reduce your pain considerably, improve your mobility, enable comfortable night’s sleep and generally improve your quality of life. You are unlikely to be able to squat and kneel afterwards however as the prosthesis does not restore full range of motion of the knee.
A knee replacement should reduce your pain considerably, improve your mobility, enable comfortable night’s sleep and generally improve your quality of life. You are unlikely to be able to squat and kneel afterwards however as the prosthesis does not restore full range of motion of the knee.
What’s involved?
Once you have decided to proceed with surgery your surgeon will arrange for pre operative investigations usually organised through pre admission clinic at the hospital. You will need to cease all anti inflammatory drugs and naturopath/herbal medicines 10 days beforehand. Ensure that you have no dental or other medical conditions that may affect outcome of surgery. You may be referred to a general physician. Cease smoking 6 weeks beforehand.
Dr Stening prefers to perform the knee replacement using patient specific instrumentation for most patients unless there is a specific reason otherwise. This is to ensure the knee replacement is well aligned. A CT scan will be arranged beforehand and information from this is used to manufacture the templates used at the time of surgery. Dr Stening can discuss this technique in more detail with you at the time of consultation.
You will usually be admitted to the hospital on the day of your surgery unless you are first on the list in which case the hospital admissions department may organize for you to come in the night before. You will meet the anaesthetist and nurses who will ask you certain relevant questions and the operative area will be shaved and cleaned. There may some more tests organised if deemed necessary.
It is important that you bring in all relevant Xrays as these will be referred to by your surgeon during the procedure.
Post-Operative Information
Post operatively you will be transferred to the recovery ward. You will have monitors attached and intravenous lines to administer medications. You may also be catheterised. An Xray will be done in recovery to check that the knee replacement is satisfactorily aligned.
On the day following your surgery the drains will usually be removed, you will be sat out of bed and physiotherapist will see you to assist with your mobilising. You will be able to put all your weight on your leg but you will be using aids such as forearm support frame or crutches to assist your walking. Approximately 3 – 5 days post operatively you will either be transferred to a rehab facility or discharged directly home depending on your home circumstances and progress while in hospital.
The timing for post operative visit with your surgeon will be arranged prior to discharge. Usually dissolvable stitches are used so there is no need for removal however you should have a wound check by either your surgeon or local doctor at 2 weeks.
Precautions
- Any cuts or scratches on the operated leg need to be dressed adequately to avoid potential infection. If you are having any dental work or other surgical procedures you should advise the surgeon that you have a knee replacement and you should receive antibiotics before and after treatment in order to prevent infection in your replacement.
- As with any major surgery there are risks and complications that may occur.
- General risks are those with the anaesthetic and others due to associated medical conditions. These include allergic reactions to medications, heart attack, pneumonia, stroke, urinary tract infection, renal failure, blood loss requiring transfusion.
- Specific risks associated with the procedure include deep venous thrombosis (DVT), stiffness, nerve damage, wound complications and deep infection. The surgical team is very mindful of these risks and measures are taken to reduce the chance of these occurring but cannot be guaranteed. If concerned you should talk to your surgeon, however a further consultation may be required.
- The prosthesis particularly the plastic insert may also eventually wear out and require revision but generally 80-90% replacements last 15 years. It is important to have occasional Xrays over the years to assess for this.
- It is particularly important to have ongoing physiotherapy either as an outpatient or whilst in rehab after discharge from hospital to minimise the risk of stiffness. Dr Stening will review you 6 weeks post operatively to check the knee is moving satisfactorily. The goal is to achieve at least 90 degrees knee flexion by 6 weeks. If this isn’t the case then a manipulation under anaesthetic followed by more physiotherapy may be necessary.
- You will also notice an area of numbness along the outer aspect of the wound. This is unavoidable and quite normal after a knee replacement. It generally doesn’t concern patients as it largely resolves.
The knee
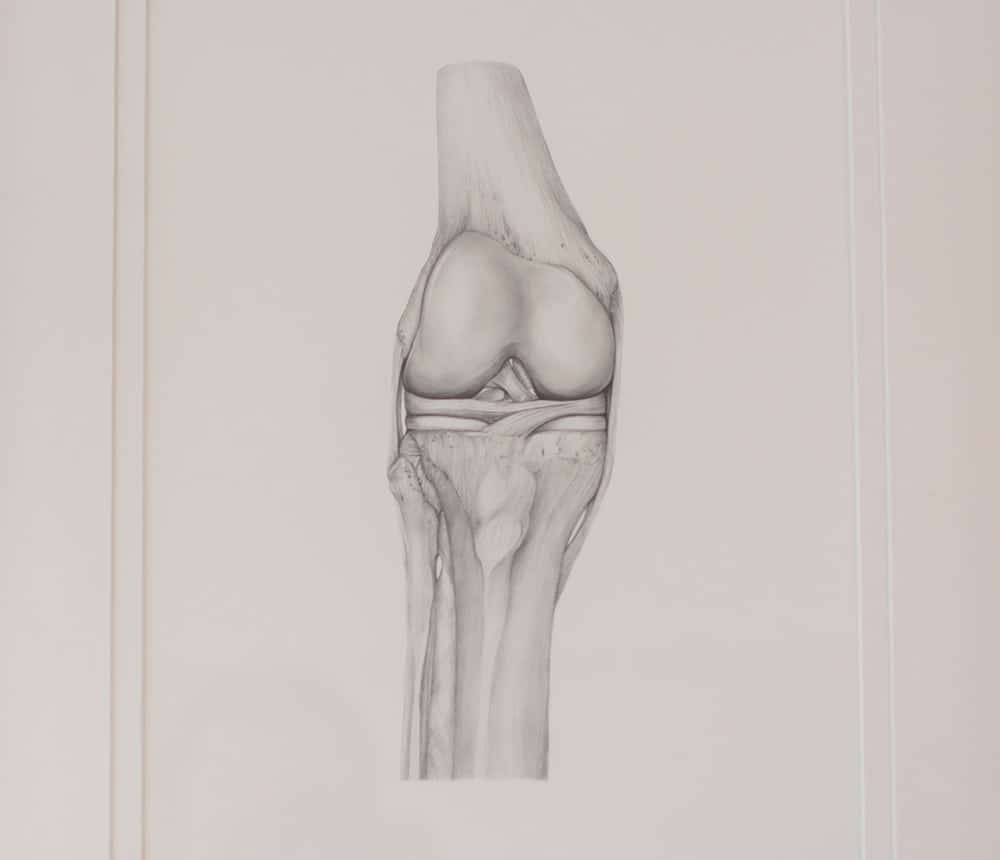
The knee is the largest and most complex joint of our body, which is held together by muscles, tendons and ligaments. It has a very hard job: carrying our body weight and enabling gait function for our entire life. Thus, it is not surprising that knees are the joints which are the most vulnerable to injuries or to develop degenerative joint diseases, such as osteoarthrosis of the knee joint.
One of the consequences of any joint disease is pain. It is very common and affects major parts of the population over 45 years of age. Statistics show that roughly one third of the American population over the age of 45 suffers knee pain. Knee pain limits your daily activities, affects your mood, your health, your general well-being, activity level and expectations. Knee pain and stiffness caused by advanced osteoarthrosis is severely limiting and your physician may suggest you undergo a total knee replacement.
The knee joint is comprised of three bones: the thigh bone (femur), the shin bone (tibia) and the kneecap (patella). When you flex or straighten your leg, the thigh bone turns on the shin bone, while the kneecap runs along the end of the thigh bone. The leg movement is driven by the thigh muscles, the biggest one being the quadriceps, located in the front of the thigh. The thigh and shin bones are connected by ligaments, which give stability to the knee joint. The surface of the kneecap, thigh bone and shin bone, where the bones come in contact, is coated with a smooth tissue called articular cartilage. The cartilage, together with a substance called synovial fluid, prevents the bones from rubbing against each other and causing damage.
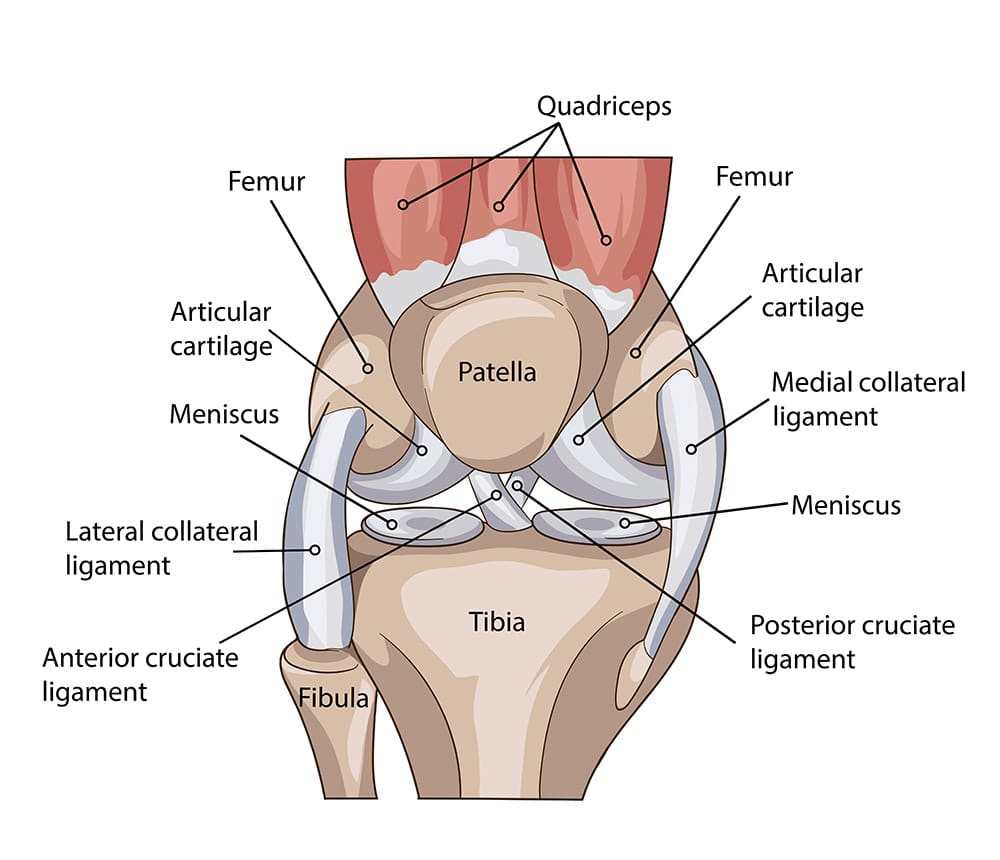
The human knee can suffer from various conditions and diseases. Untreated these conditions can result in degenerative changes of the knee joint causing pain and loss of function. Osteoarthritis is the most common form of the degeneration of the knee joint. The main cause is the wear of the articular cartilage. This wear causes pain, initially only when a load is bearing on the joint but over time it becomes painful more and more frequently eventually leading to constant pain even when resting. The increase in intensity of the pain is a slow process, sometimes over many years, and can lead to a stiff knee joint. Successful knee replacement can result in dramatic pain relief and improvement in the knee joint function.
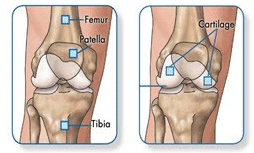
Researchers are not exactly sure what causes knee osteoarthritis, but evidence shows what may cause this condition. It may actually be that a variety of factors can lead to the wear and tear of your knee cartilage. Generally, most degenerative changes of the knee joint are contributed by:
- Age: Most people who have osteoarthritis are older than 45 years old.Your age puts you at risk for developing knee osteoarthritis. Throughout daily life, you put your knee joints through a lot of stress, and your cartilage can start to wear down over time.
- Gender: Women are more likely than men to develop osteoarthritis, especially in people who are older than 45 years old.
- Genetics: Knee osteoarthritis may be hereditary: If a family member has osteoarthritis, you could be at greater risk of developing it, too.
- Previous Injury: If you’ve ever had a knee injury, especially cartilage, meniscal or ligament damage that required surgery, you could be more prone to getting knee osteoarthritis.
- Obesity: Carrying around too much extra weight can put strain on your knee joints, making the cartilage wear out quicker than it normally does. Reaching and maintaining a healthy weight can help prevent knee osteoarthritis or reduce its symptoms. If you already suffer knee osteoarthritis, a healthy weight can help prevent it from progressing.
- Overuse: Certain sports (eg, soccer), overuse and repetitive stress of your knee joints can put too much strain on the cartilage in your knees, causing premature breakdown.
These are some of the most common causes of knee osteoarthritis. However, sometimes knee osteoarthritis can develop without any obvious cause. If you’re concerned that you could be at risk for developing knee osteoarthritis, please talk to us right away.
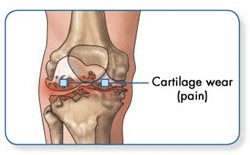
Knee osteoarthritis tends to develop gradually. It may take some time for your cartilage to wear down, which may result in just slowly increased symptoms of knee osteoarthritis over a long period of time. However, it’s possible (but not as common) for knee osteoarthritis to develop suddenly. You may experience knee osteoarthritis in one or both of your knees. Commonly, pain isn’t the only symptom of knee OA. Below are some of the most common knee osteoarthritis symptoms.
- Pain: Pain is a classic symptom of knee osteoarthritis. The pain can make your knee feel sore and achy, weak or wobbly, or as if it will lock in place. Knee pain may be more intense when you move your knee. Over the course of time, you may need more and more periods of rest during sports or even daily activities. It might be more noticeable after using the knee joint too much or after periods of being inactive.
- Swelling and stiffness: Stiffness is a common symptom that can make the knee joint feel as if it is hard to bend or straighten. Fluid in the knee joint can accumulate, which can cause it to look swollen. If swelling and stiffness do not improve with rest or medications, it’s a good idea to see us.
- Restricted movement: As the knee osteoarthritis gets worse, it can cause limited movement in the joint that can make it hard to do simple tasks, such as climbing stairs, walking to the mailbox, or getting in and out of bed.
Symptoms such as pain and stiffness are often worse in the morning or after being inactive, while swelling usually occurs after a long period of excessive activity. Changes in the weather, when it’s rainy and/or cold, may also make the pain and other knee OA symptoms feel worse. Not everyone with knee osteoarthritis has the same symptoms. But if you experience any of the symptoms of knee osteoarthritis, please talk to us right away. It’s important for you to get the appropriate treatment for knee osteoarthritis.
Surgery is typically a last resort for knee osteoarthritis. Before knee replacement surgery, alternative treatment options, such as medications, physical therapy, exercise and less invasive surgery can be suggested.
There are many treatments available for knee osteoarthritis. We will work with you to develop a treatment plan that is appropriate to reduce your specific symptoms, especially the pain and trouble moving.
Complementary and alternative treatments include:
- Acupuncture: Stimulates different anatomical points on the body using very fine needles. You may also want to try massage or other forms of physical therapy.
- Exercise: Although it may sound painful and counter-productive, exercise can help improve your range of motion in your knee. Also, if you currently exercise but the type of exercise you do, such as running, increases your pain, you will probably need to switch to a more low-impact exercise, such as swimming. A physical therapist can help you develop an exercise plan that works for your life, as well as learn how to move in ways that don’t increase your pain. In addition to exercise, you may also need to undergo other physical therapy treatments for knee osteoarthritis.
- Injections: This treatment option improves knee joint lubrication by injection of hyaluronic acid (a substance found in synovial fluid) into the knee. The substitute may help, because in osteoarthritis, you can lose the synovial fluid that lubricates the joint. Also, a steroid injection may help reduce pain by controlling the inflammation of the knee joint.
- Weight loss: Being overweight can put extra pressure on your knees. If you have extra weight, we will develop weight loss programs in collaboration with a dietician that will support you to lose it thoughtfully.
- Medications: An over-the-counter analgesic (painkiller), such as Panadol, can help reduce your pain. If you want a medication that addresses the pain and the inflammation of knee osteoarthritis, you may want to try a non-steroidal anti-inflammatory drug (NSAID). If you tend to use painkillers on a frequent basis, please discuss the medication with us. You should keep in mind that all medications used for knee osteoarthritis treat the pain and symptoms, but they aren’t curing the knee osteoarthritis.
If you’ve tried non-surgical treatments for several months, and they are not good enough to cope with the pain, swelling, stiffness, and other symptoms of knee osteoarthritis, we may initially suggest minor-invasive surgical options depending on the grade of osteoarthritis, your activity level and age. The goal of these surgical options for knee osteoarthritis is to help you return to your normal activities without major rehabilitation. After recovering from surgery, you may notice you’re able to move more easily, and you may feel less pain and swelling in your knee joint.
- Arthroscopy: This procedure is less invasive than joint replacement because we just use a tiny incision to work with a small camera, small instruments and tools during surgery. Generally, we will clean up your knee joint by removing any debris (damaged cartilage or tissue) to prevent further joint deterioration. Although arthroscopy may sound more desirable than total knee replacement, it’s often not the best option. It depends on the progression of your osteoarthritis. Talk to us about whether arthroscopic surgery is an option for you.
- Osteotomy: An osteotomy is a surgical intervention where a part of the bone is removed to improve alignment of the knee. It has a prolonged rehabilitation time.
We will take into account whether you’re a candidate for these kinds of knee surgeries: your age, occupation, severity of pain and other symptoms, and the degree to which arthritis interferes with your daily activities. However, the decision to have surgery for knee osteoarthritis is ultimately up to you.
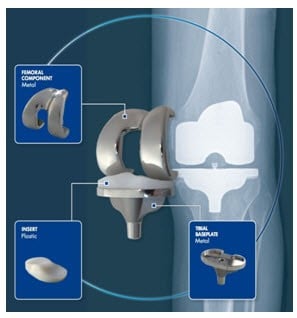
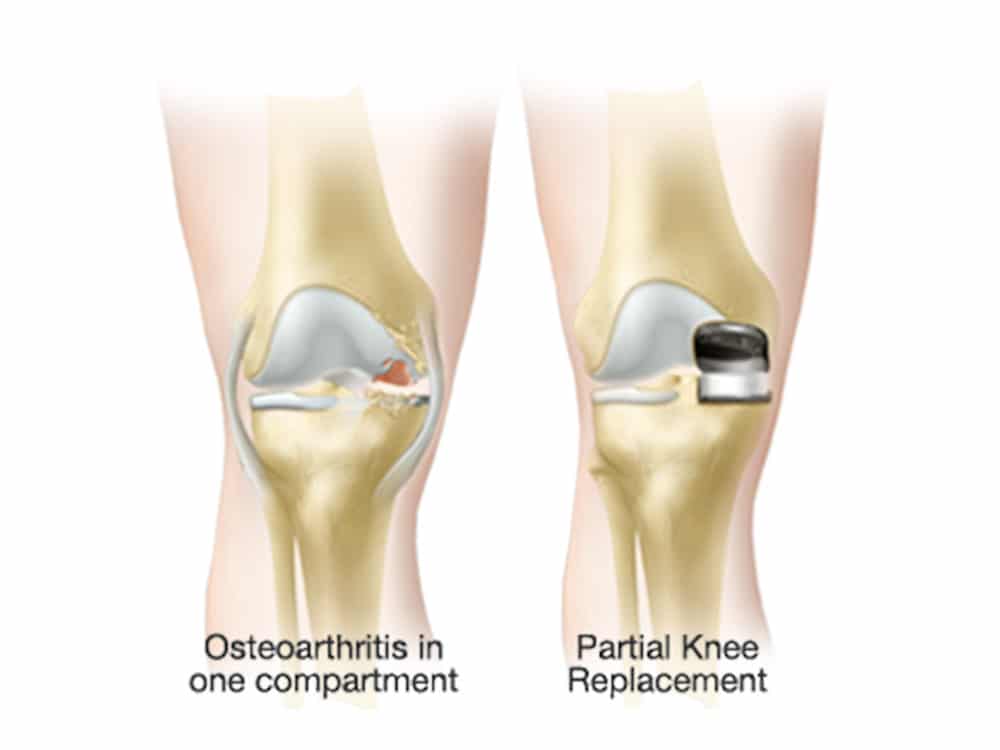
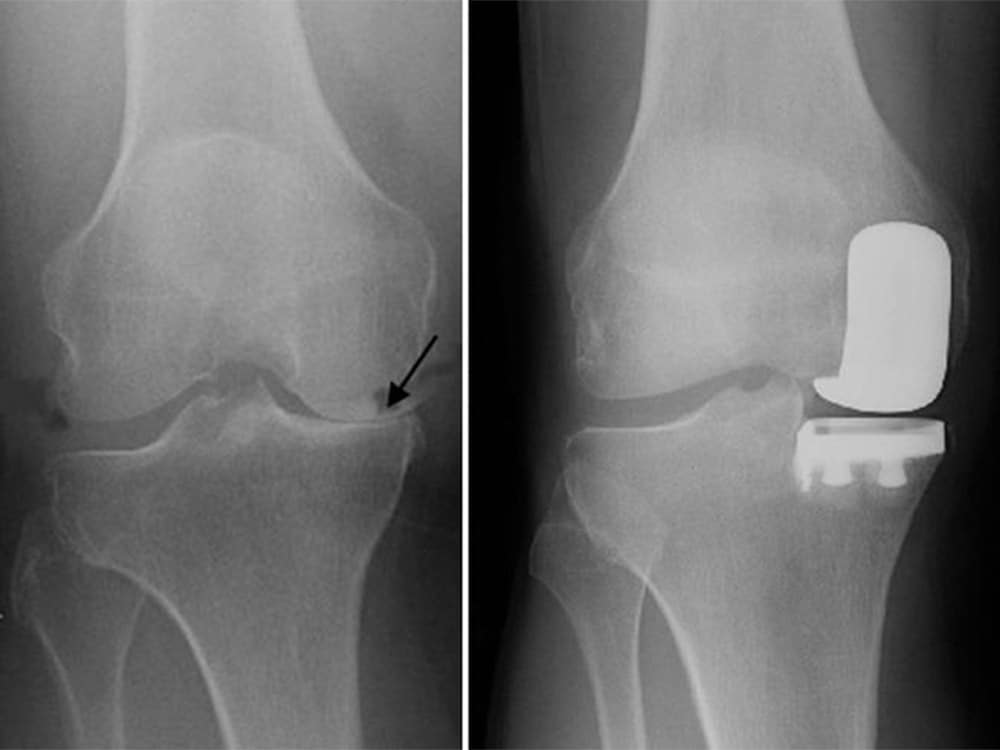
Knee replacement is typically the last resort for knee osteoarthritis after surgical and non-surgical treatment options have failed and you are still suffering increasing pain and loss of function. We replace all of the damaged cartilage in the knee joint (called total knee arthroplasty) or just a part of the joint (called partial knee arthroplasty) using artificial parts. Total knee replacement surgery aims at substituting the bone and cartilage of the joint damaged by arthritis with plastic and metallic components. The surfaces of the thigh and shin bones are replaced with high-resistant metallic components, called the femoral component and tibial baseplate. Between the femoral component and the tibial baseplate, a plastic insert is implanted. It replaces the cartilage function allowing the thigh and shin bone to slide on each other. All materials used in a total knee replacement are highly biocompatible.
With almost 50 years of history, total knee replacement surgery is a very common and safe procedure for the treatment of severe arthritis. Approximately 1,000,000 knee replacements are performed annually worldwide. The main benefits of a successful total knee replacement are:
- Reduction of pain. The pain may be rapidly and dramatically reduced, usually eliminated.
- Recovery of mobility. With less effort, you may regain close to the original mobility of your knee.
- Improvement of quality of life. Your everyday activities and your social life may no longer be limited by pain and reduced mobility.
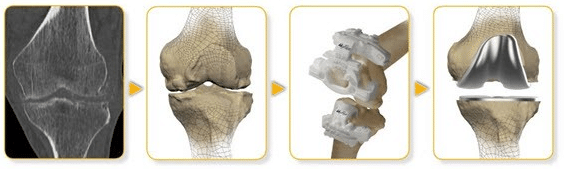
The positioning of knee prosthesis is achieved using special surgical instruments which prepare the bone for implanting the prosthesis (cutting blocks). When planning and performing a total knee replacement for patient surgeons have several options.
Conventionally, surgeons tended to use 2 dimensional X-ray images and a transparent template to decide about the size and placement of the artificial knee components. In conventional procedures the surgical instruments are the same for all patients. Also, conventional instrumentation doesn’t allow the surgeon to tailor the surgical procedure to each patient specifically. Depending on surgeon’s experiences, studies have shown that conventional knee replacement procedures is sometimes less precise than the preoperative planning.
To improve precision, a new technique is now available, which is called MyKnee. This new approach to preoperative planning utilizes 3 dimensional CT images to provide the surgeon with a customized, 3D template and instruments for every patient prior to surgery. MyKnee customizes knee replacement surgery to each and every patient. CT images of the patient’s knee are sent electronically to the manufacturer of the artificial components to analyze and design a cutting guide from the exact specifications of the patient’s knee. The preoperative plan is then sent electronically back to the surgeon for final approval. Once approved, Medacta creates the customized cutting guides for that particular patient’s knee in Switzerland and sends it along with the appropriate surgical tools to the surgeon for the procedure. MyKnee® is a surgical instrument which fits the patient’s knee accurately, because it is custom made. As a consequence MyKnee technology potentially assures the following results
- More accurate positioning of the prosthesis. MyKnee® fits the shape of the knee accurately, allowing precise preparation of the bone for implanting the prosthesis. Each phase of the operation is planned by the surgeon prior to the operation by analysis of a tridimensional model of the knee and taking the patient’s condition into account. It has been proven that an accurate positioning results in increased survival of the prosthesis
- Improved balance and stability of your knee ligaments
- Less traumatic procedure. Conventional procedures require damaging anatomic structures (e.g. medullary canal) in order to position the surgical instruments used to implant the prosthesis. MyKnee® preserves these structures, allowing a dramatic decrease of blood loss and risk of embolism
- Faster operation. The use of the MyKnee® technology is very simple and straightforward. It potentially allows the surgeon to reduce the operating time, thus decreasing the time under anesthetic and the risk of infection[
The MyKnee® technology allows for a more accurate, faster and less traumatic total knee replacement, by the use of a surgical instrument tailored for the patient.
If you decide to have a total knee replacement using MyKnee patient matched technology, we will ask you to have a diagnostic CT scan of your leg. Medacta® will create a plastic 3-dimensional model of your knee using the image from the diagnostic scan in order to help the surgeon select the best implant for you. Using the model of your knee, Medacta®, together with your surgeon, creates your personalized surgical instrument. Prior to the surgery, your surgeon will receive the MyKnee® instruments and a plastic replica of your knee. This will be analyzed by your surgeon to prepare accurately for your knee operation. The MyKnee® technology allows for a more accurate, faster and less traumatic individual total knee replacement, by the use of a surgical instrument tailored precisely for your knee.